Nail Trauma & Pressure Injuries
By the end of this lesson, the learner will be able to:
- Differentiate acute traumatic nail injuries from chronic microtrauma from poorly fitting footwear.
- Recognize subungual hematoma and apply appropriate triage criteria for escalation versus routine management.
- Describe the typical timeline of nail regrowth and counsel patients accordingly.
- Identify the most common footwear-related pressure points and teach prevention strategies.
Not every black, lifted, or bruised toenail is a fungal infection — many are the result of trauma. Acute injuries (a dropped object, a stubbed toe) and chronic microtrauma (poorly fitting shoes during long runs or hikes) both produce visible nail changes that look alarming but are usually benign. This lesson covers what to look for, when to escalate, and what to teach so the next nail comes in healthy.
Acute Trauma vs. Chronic Microtrauma
The two mechanisms produce similar-looking nails but call for different teaching. Identifying which one you're seeing is the first step.
Always ask about footwear and recent activity when a patient presents with a "fungal" or discolored nail. A surprising number of "onychomycosis" cases are actually chronic microtrauma — and antifungal treatment will fail if the cause is the patient's shoes.
Subungual Hematoma: A Decision Pathway
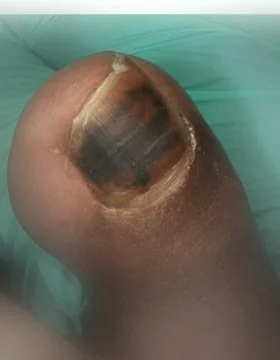
A subungual hematoma is a collection of blood beneath the nail plate — usually from acute trauma but sometimes from chronic microtrauma. The key nursing question is whether the patient needs urgent evaluation or routine management.
- Dark red, purple, or black discoloration
- Throbbing pain (acute)
- Pressure sensation under the nail
- Tenderness on palpation
- Severe, throbbing pain not relieved by elevation
- Hematoma covers more than ~25% of the nail
- Suspected fracture (deformity, crepitus, severe focal tenderness)
- Nail bed laceration or partial avulsion visible
- Patient with diabetes, peripheral vascular disease, or immunocompromise
- Anticoagulation or bleeding disorder
- Crush mechanism suggesting deeper injury
- Cool compresses and elevation in the first 24–48 hours
- Acetaminophen for pain control as appropriate
- Protect the nail; keep clean and dry
- Educate the patient: the nail will likely lift and may eventually fall off as a new nail grows in
- Counsel on footwear fit if the cause was microtrauma
- Return to clinic if pain worsens, signs of infection appear, or the nail bed becomes exposed
You may have seen videos of "draining" a subungual hematoma by piercing the nail plate. This is a procedural intervention performed by a qualified provider, not a nursing intervention. The nurse's role is recognition, triage, comfort measures, and escalation when indicated.
The Nail Regrowth Timeline
One of the most useful things a nurse can give a patient with a nail injury is a realistic timeline. A toenail grows roughly 1–2 millimeters per month — about half the speed of a fingernail.
Patients are often distressed when a damaged toenail begins to lift weeks after an injury — they think something is going wrong. Telling them up front that this is expected, and that the new nail will take roughly a year to fully replace the old one, prevents unnecessary anxiety and unnecessary visits.
Footwear Pressure Points
Most chronic nail trauma comes from footwear that's too short, too tight, or too loose. Three pressure mechanisms account for almost all chronic nail injuries.
Three pressure mechanisms
Partial & Complete Avulsion
When the nail plate partially or completely separates from the nail bed, management depends on whether the bed is exposed and whether infection risk is elevated.
- Loose or partially detached nail plate
- Exposed nail bed (in complete avulsion)
- Bleeding
- Variable pain
- Clean the area gently and apply a non-adherent dressing
- Do not forcibly remove a still-attached nail; trim only loose, sharp fragments that risk further injury
- Coordinate provider evaluation when bed is exposed, bleeding is significant, or the patient is high-risk
- Educate the patient: a new nail will grow in over 9–12 months
- Tetanus status review per institutional protocol if mechanism warrants
Patient Education for Trauma Prevention
Ask the patient when they last bought new shoes and have them stand in their current pair. Confirm there's a thumb's width of space between the longest toe and the front of the shoe. Check that the heel doesn't slip and the instep isn't compressing the dorsum. Recommend trying on shoes at the end of the day when feet are at their largest, and replacing athletic shoes every 300–500 miles or every 6–12 months. This conversation prevents more nail problems than any topical treatment.
Ready to check your understanding? Take the quick knowledge check for this lesson.
The information on this website and any communication with RNscrub Foot Care is provided for educational and informational purposes only. It is not a substitute for medical advice, diagnosis, or treatment. Patients are always encouraged to consult with their primary care provider or appropriate specialist for individual clinical decisions.
References
- Tully AS, Trayes KP, Studdiford JS. Evaluation of nail abnormalities. American Family Physician. 2012;85(8):779–787.
- Pingel C, McDonald SE, Almasi P. Nail trauma in athletes. Sports Health. 2017;9(5):422–428.
- Kayalar M, Bal E, Toros T, et al. Crush injury to the distal phalanx with subungual hematoma. The Journal of Hand Surgery. 2011;36(2):236–241.
- Wound, Ostomy and Continence Nurses Society. Core Curriculum: Wound Management. 3rd ed.
- Habif TP. Clinical Dermatology: A Color Guide to Diagnosis and Therapy. 7th ed. Elsevier; 2021.
- de Berker D. Nail anatomy. Clinics in Dermatology. 2013;31(5):509–515.

